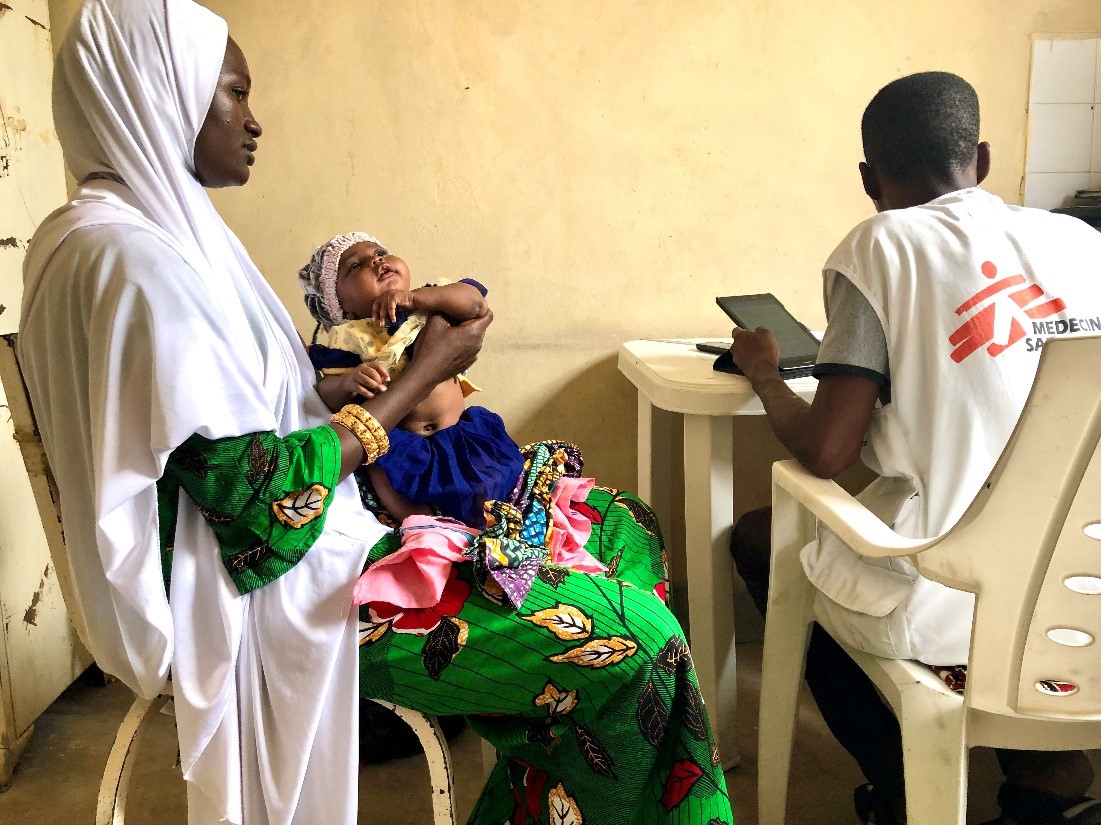
Improving Patient Care with an electronic Decision Support System (EDSS)
MSFeCARE is designing, implementing, and scaling a tool to provide frontline clinicians with guided decision-making support to increase the quality of clinical assessment and care.

Tell us about the problem you are trying to solve.
With very limited access to diagnostic tools and often overwhelming patient case loads, frontline health workers in low-resource settings struggle to provide high quality care to their patients. Consultations are often rushed or sub-optimal, leading to inaccurate diagnoses and unnecessary or incorrect prescriptions. This in turn hampers the clinical outcomes of patients and reduces trust in the overall health system. Health workers need support to improve their clinical assessment and diagnostic skills, which is a prerequisite to improving rational and evidence-based antibiotic prescriptions and patient care.
Our objective is to improve the quality of care for patients and foster the autonomy of frontline health care workers through guided decision-making, evidence-based diagnostics and prescription, enhanced learning processes, and clinical supervision.
What is your solution and what motivates you to work on addressing this problem?
We have developed MSFeCARE-Ped, an electronic Decision Support System (eDSS) for pediatric primary care. Medical field workers use a mobile tablet to go through a series of questions during a patient consultation. The result is a comprehensive diagnosis coupled with treatment recommendations. The software algorithms were developed by MSF and external medical experts based on fact-based evidence and targeted to MSF low-resource contexts. The tool applies new ways to support a patient-centered consultation process at the point of care. Using an eDSS ensures attractive learning opportunities for health workers, correct applications of up-to-date evidence-based protocols, and real-time data collection, which is fed back directly to the health facility for continuous and iterative self-improvement.
“A mother came out of the consultation with only paracetamol and was given some advice. She was not very happy, but the health educator explained to her that antibiotics were not always necessary. Two days later, she returned to us very happy as her child had recovered without the need for more medication thanks to MSFeCARE”.
– Flying MSFeCARE Implementer – Ngoc-Thu, Kabo, CAR, CDS Kabo.
This project has a strong transformational dimension for MSF and beyond:
- Our patients benefit from improved consultations and better interaction with patients.
- Our front-line field workers based even in the most remote contexts are supported through guidance and supervision and can integrate new competencies and expertise in their clinical roles.
- The community as a whole benefits from improving rational antibiotic prescriptions, and limiting its negative impact on the development of antibiotic resistance.
- Evidence generated through the data collected in eDSS-interventions can continuously improve MSF operations and clinical support.
- MSF can adapt eDSSs developed internally or by other actors and share its own intervention models and tools including successes and failures.
- New areas of medical care can be applied by expanding the tool to other contexts.
What have you done so far and what results have you achieved?
MSFeCARE-Ped is currently deployed in 8 MSF projects, in 6 countries: Mali, Niger, Chad, Kenya, Central African Republic (CAR), and Tanzania.
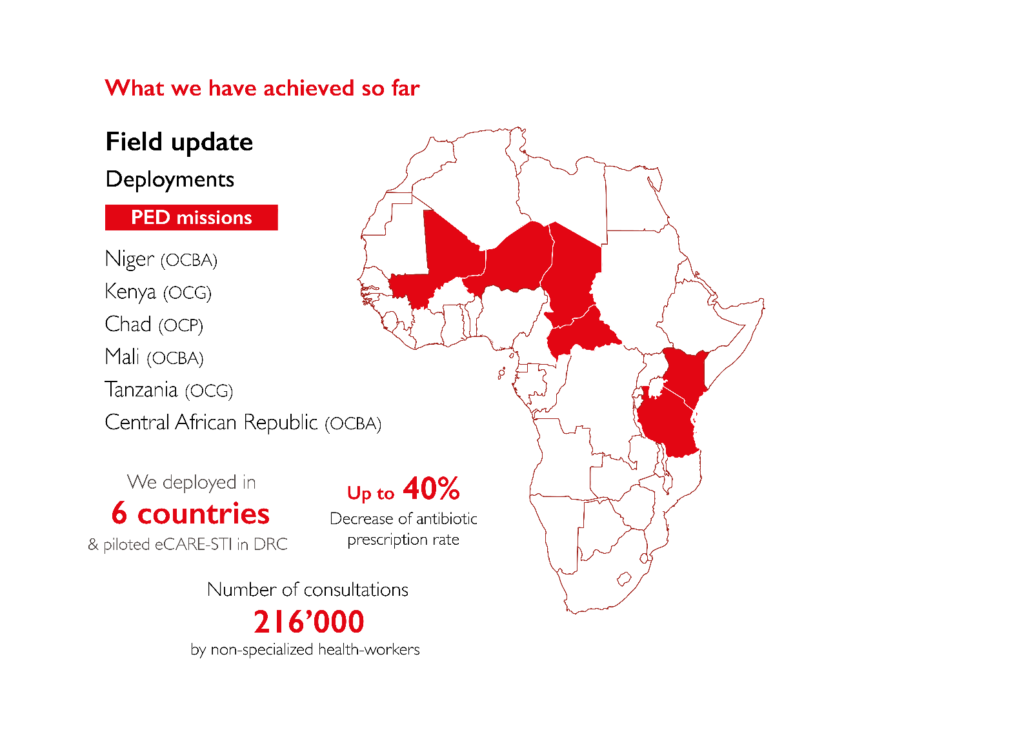
MSFeCARE eDSSs created:
- PED (Pediatric) was the first eDSS created, today it is deployed in 6 countries.
- STI (Sexually Transmitted Infections) was the second eDSS created and was piloted in DRC in 2019.
- COVID-19 was the most recent eDSS created and is currently being finalized.
What have staff said about the project?
“MSFeCARE allows nurses to take fast decisions for patient management especially for emergency cases.”
– Elhadj Diop, Medical Team Leader, Diffa, Niger
“There are questions that we were not asking before, or not in all consultations. Now with eCARE it is systematic, we have to ask the questions.”
– Ali Saibou Djaouna, Nurse, Diffa, Niger.
“It brings a good relationship between diagnostic and prescription – it reduces the over-prescription of antibiotics.”
– Cécile Nato, Nurse Activity Manager, Diffa, Niger.
How has your project pivoted to support MSF’s response to the COVID-19 pandemic?
The COVID-19 pandemic represents an unprecedented situation where MSF’s expertise in dealing with epidemics can make a huge difference. It also challenges MSF’s way of working, in particular, by limiting its capacity to send field workers to our projects. In these times of restricted travel, digital tools can help to share expertise and collect information for a variety of fields, like epidemiological surveillance, triage, case detection, contact tracing, and health facility- or home-based case management. Digital tools can also provide user-friendly ways to support health care workers facing stressful situations.
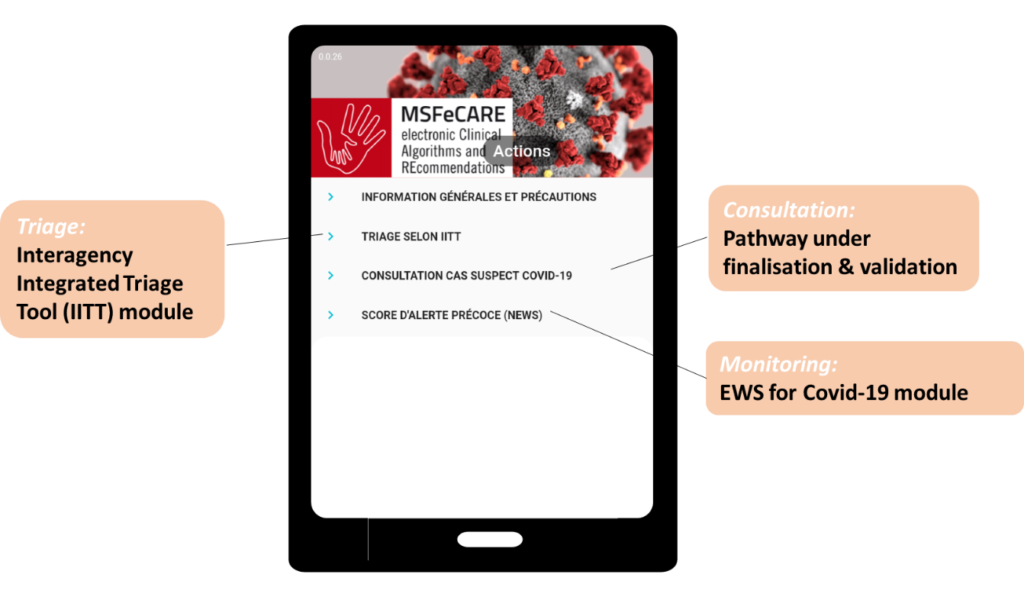
The MSFeCARE team identified 3 key activities where clinical decisions support tools could help health workers quickly understand and apply the new guidance develop by experts:
I.Triage
When there is a critical influx of patients to a health facility, a proper triage system is crucial to ensure patients are seen according to priority of their illness. Severe cases that require immediate life-saving treatment and care are responded to first. To support this, a digital triage module has been developed, based on the Interagency Integrated Triage Tool, developed by MSF, ICRC, and the WHO, and currently recommended for triage in MSF projects by the Emergency Medicine and Critical Care working group (EMACC-WG).
II.COVID-19 Case Management
Once a patient is identified as a suspected, probable, or confirmed COVID-19 case, the health worker must determine the severity. Based on their assessment, they must decide on initial treatment, level of care required, and monitoring. As a new disease, management guidelines and evidence for COVID-19 are frequently updated, making it challenging for health workers to understand and correctly apply the recommendations, especially under the particularly stressful pandemic conditions.
To support user adoption, OCG’s case management protocol was transformed into a digital decision algorithm. This algorithm helps clinicians navigate through the complex management protocol and to helps them check how the rules apply to their patient’s specific clinical needs.
III. Hospital Monitoring
To support health workers in rapid diagnosis and treatment , a few clinical scores have been developed and evaluated. The NIH Early Warning Score (NEWS), developed by the UK Royal College of Physicians, has substantial evidence to predict deterioration, and is recommended by the EMACC-WG for COVID-19 cases.
A simple NEWS calculator has been developed as a module in the MSFeCARE-COVID-19 application.
The 3 modules described above have been integrated into a MSFeCARE-COVID-19 app. This app does not collect any patient data.; Field health workers can download the app to their own devices and use for self-training, or to confirm patient-related decisions. Updates can be disseminated quickly to the mobile app.
What challenges have you faced?
The dedicated clinicians we work with face heavy patient case loads without specialized training or adequate diagnostic resources. Finding the right balance between improving the quality of primary care pediatric consultations and keeping the implementation feasible in high-workload projects is one of our biggest challenges. The increase in consultation time is also frequent concern, but after proper training and practice, our past deployments have demonstrated that this balance can be achieved.
Staff turnover in unstable MSF projects is another critical challenge. Having trained staff who feel comfortable with using the application is key, but constant turnover makes it difficult to reach all staff. With this in mind, we are working to develop simplified training and implementation kits and assessing remote learning opportunities.
What lessons have you learned?
We’ve learned that employing various health promotion and community awareness strategies before and during deployments is very important. If the affected community understands the goals of our project, they are more likely to accept lower antimicrobial prescription rates or longer waiting time for adults for the benefit of children. Clinicians will be able to adopt the tool and improve the quality of care successfully. In addition, allocating enough time and resources to clinical supervision of Out-Patient Department (OPD) health workers is key. Finally, MSFeCARE provides new tools and a supporting environment for supervision, but regular supportive supervision sessions and peer support in the health facilities are still needed.
What is next?
After the success of the pilot missions, MSF’s Executive Committee approved a TIC proposal to launch the MSFeCARE programme, a 3-year large-scale initiative with support from Operational Centers Geneva, Barcelona and Paris. The mandate of the programme can be simply described in the graphic below.
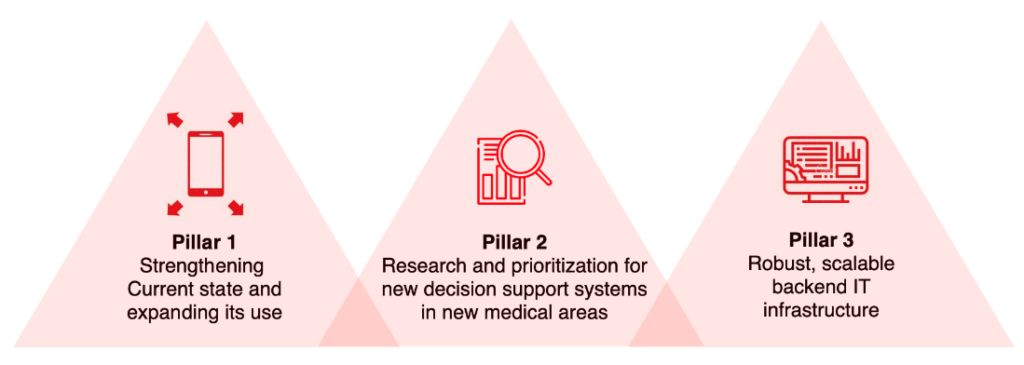
This programme will enable us to scale up MSFeCARE-Ped and other eDSS tools that we will build wherever relevant. The investment in this project will have a transformational impact on our field staff and will markedly improve the quality of care for our patients where it is needed the most.
Are there any interesting partners that you are collaborating with?
We have engaged with Things Prime and used their platform, Logiak, to digitalize the algorithm for MSFeCARE-Ped. We are also part of a collaborative effort with Terre des Hommes, ICRC, Swiss TPH, FIND, WHO to disseminate lessons learned in digitalizing paediatric clinical protocols, which are supported by the Geneva Health Forum and the Geneva Science Policy Interface.
In addition, we are also beginning to actively participate in the MSF International Paediatric Working Group to help us in the process of reviewing and updating the current Ped version of MSFeCARE. And finally, we are collaborating with MSF Academy to develop a curriculum that will harness the use of MSFeCARE to strengthen the clinical reasoning capacity of Out-Patient Department (OPD) hospital nurses.
What is the expected long-term impact of the project? How will this project improve MSF’s lifesaving work?
 Our goal is to improve the quality of care and ultimately save lives in remote settings by guiding health care workers in decision-making through evidence-based diagnostics and prescriptions, enhanced learning processes, and clinical supervision.
Our goal is to improve the quality of care and ultimately save lives in remote settings by guiding health care workers in decision-making through evidence-based diagnostics and prescriptions, enhanced learning processes, and clinical supervision.
By implementing this program, we expect to:
- Widely expand the use of MSFeCARE-Ped with robust M&E protocols to more missions and countries and a wider network of health care workers;
- Create a new eDSS in a new medical area to extend the model into medical sectors that can benefit from a decision-making tool, equipping health workers already experienced with MSFeCARE with new skills and/or increasing the number of health care workers using MSFeCARE;
- Inspire the use of eDSS beyond medical interventions in other areas of MSF’s work.
For more information on this project, please reach out the MSFeCARE project team at anteia.win@geneva.msf.org.